Tagged / Nepal
Happy New Year!
We are wishing our colleagues, students, researchers and collaborators from South Asia a Happy New Year today. The best wishes for the Bangla New Year 1433 and for the Nepali New Year 2083!
Professors Edwin van Teijlingen and Vanora Hundley

New academic paper on Nepal
Yesterday the international journal Health Policy & Planning published our latest article with the title ‘Understanding the formulation of non-communicable disease policies in Nepal: A qualitative study‘ [1]. The paper is part of the PhD work (at the University of Hudderfield) by the first author, Dr. Anju Vaidya, who is originally from Nepal. Anju’s thesis was supervised by Prof. Padam Simkhada (University of Chester), Prof. Andre Lee (The University of Sheffield) and by Bournemouth University’s Prof. Edwin van Teijlingen.
The paper recognises that there is limited evidence about the process through which health policies were formulated in Nepal. This study used Kingdon’s multiple streams framework to explore how NCDs (non-communicable diseases) were recognised and prioritised, how policy alternatives were decided, how policy windows were opened, and which contextual factors influenced the policy formulation process. Anju’s PhD included a qualitative study to gain a comprehensive understanding of the formulation of major NCD-related policies in Nepal. Semi-structured interviews were conducted with 12 key stakeholders, and policy documents were analysed using framework analysis.
The NCDs were gradually prioritised through the convergence of global and local evidence, sustained advocacy, and international commitments. Policymakers encountered several challenges, such as competing health priorities, the chronic nature of NCDs, donor preferences for communicable diseases, financial constraints, and multisectoral complexities of NCDs. The Package of Essential Non-communicable diseases (PEN) interventions were adopted as a policy alternative, informed by global evidence, World Health Organization (WHO) recommendations, and lessons from other countries. While coordinated efforts by stakeholders brought the problem, policy and politics streams together, the role of policy entrepreneurs was found to be less relevant in Nepal’s context.
Health Policy & Planning is an Open Access journal, hence the paper is available worldwide to anybody with internet access.
Prof. Edwin van Teijlingen
Centre for Midwifery & Women’s Health
References:
- Vaidya, A., Simkhada, P., van Teijlingen, E., Lee, A.C.K. (2026) Understanding the formulation of non-communicable disease policies in Nepal: A qualitative study, Health Policy and Planning, [online first] czag048, https://doi.org/10.1093/heapol/czag048
Prof Marahatta promoting BU-Nepal collaboration
 On Monday 9th March Prof. Sujan Marahatta visited Bournmouth University (BU) to speak about ‘Strengthening BU-Nepal collaboration AND Nepal’s experience of competency-based health professional education’. Prof. Marahatta is the Director of the Medical Education Commission in Nepal overseeing the education of health professionals in 15 areas including Medicine, Physiotherapy, Nursing and Midwifery.
On Monday 9th March Prof. Sujan Marahatta visited Bournmouth University (BU) to speak about ‘Strengthening BU-Nepal collaboration AND Nepal’s experience of competency-based health professional education’. Prof. Marahatta is the Director of the Medical Education Commission in Nepal overseeing the education of health professionals in 15 areas including Medicine, Physiotherapy, Nursing and Midwifery.  He spoke about long partnership between Manmohan Memorial Institute of Health Sciences (MMIHS) and BU. This partnership is formalised in a Memoradum of Agreement (MoA) and over the years it has included joint research projects, staff-student exchanges (funded by ERASMUS+ and Turing scheme) and offering guest lectures at each others institutions.
He spoke about long partnership between Manmohan Memorial Institute of Health Sciences (MMIHS) and BU. This partnership is formalised in a Memoradum of Agreement (MoA) and over the years it has included joint research projects, staff-student exchanges (funded by ERASMUS+ and Turing scheme) and offering guest lectures at each others institutions.
One of the jointly conducted studies which Prof. Marahatta highlighted was the work on CPD (Continuous Professional Development) in nursing and midwifery in Nepal. Research on CPD started a decade ago and culminated in several papers [1-4]. The research was combined with sustained advocacy and stakeholder engagement, and resulted in the Nepal Nursing Council (NNC) formally introduced mandatory CPD as a requirement for nursing and midwifery re-registration earlier this year (15 January 2026). The National Guideline on Continuing Nursing and Midwifery Education (CNME) CPD for Nurses and Midwives refer to our work conducted by academics based at Bournemouth University. This is the foundation for one of BU’s REF Impact Case Studies for 2029.
Amongst other studies, Prof. Marahatta also highlighted a recent publication which was jointly authored between BU’s professors Clark and Hundley and himself on pain catastrophising in nulliparous women in Nepal, the importance for childbirth [5]. Prof. Marahatta’s visit was held in the Faculty of Health, Environment & Medical Sciences (HEMS) in the Bournemouth Gateway Building.

References:
- Simkhada B, Mackay S, Khatri R, Sharma CK., Pokhrel T, Marahatta SB., Angell C, van Teijlingen E, Simkhada P. (2016) Continual Professional Development (CPD): Improving Health Prospect15 (3):1-3.
- Khatri, RJ, van Teijlingen, E, Marahatta, SB, Simkhada, P, Mackay, S and Simkhada, B. Exploring the Challenges and Opportunities for Continuing Professional Development for Nurses: A Qualitative Study with Senior Nurse Leaders in Nepal. Journal of Manmohan Memorial Institute of Health Sciences. 2021 7(1):15-29.
- Simkhada B, van Teijlingen E, Pandey A, Sharma CK, Simkhada P, Singh DR (2023) Stakeholders’ Perceptions of Continuing Professional Development among Nepalese Nurses: A Focus Group Study Nursing Open.10(5).
- Simkhada B, van Teijlingen E, Sharma C, Pandey A, Simkhada P. (2023) Nepal needs Continuing Professional Development for Re-registration in Nursing and Midwifery Journal of Nepal Health Research Council, 21(60):541-42.
- Clark CJ, Marahatta SB, Hundley VA. (2024) The prevalence of pain catastrophising in nulliparous women in Nepal; the importance for childbirth. PLoS ONE 19(8): e0308129. https://doi. org/10.1371/journal.pone.0308129.
BU academics in the news in Nepal
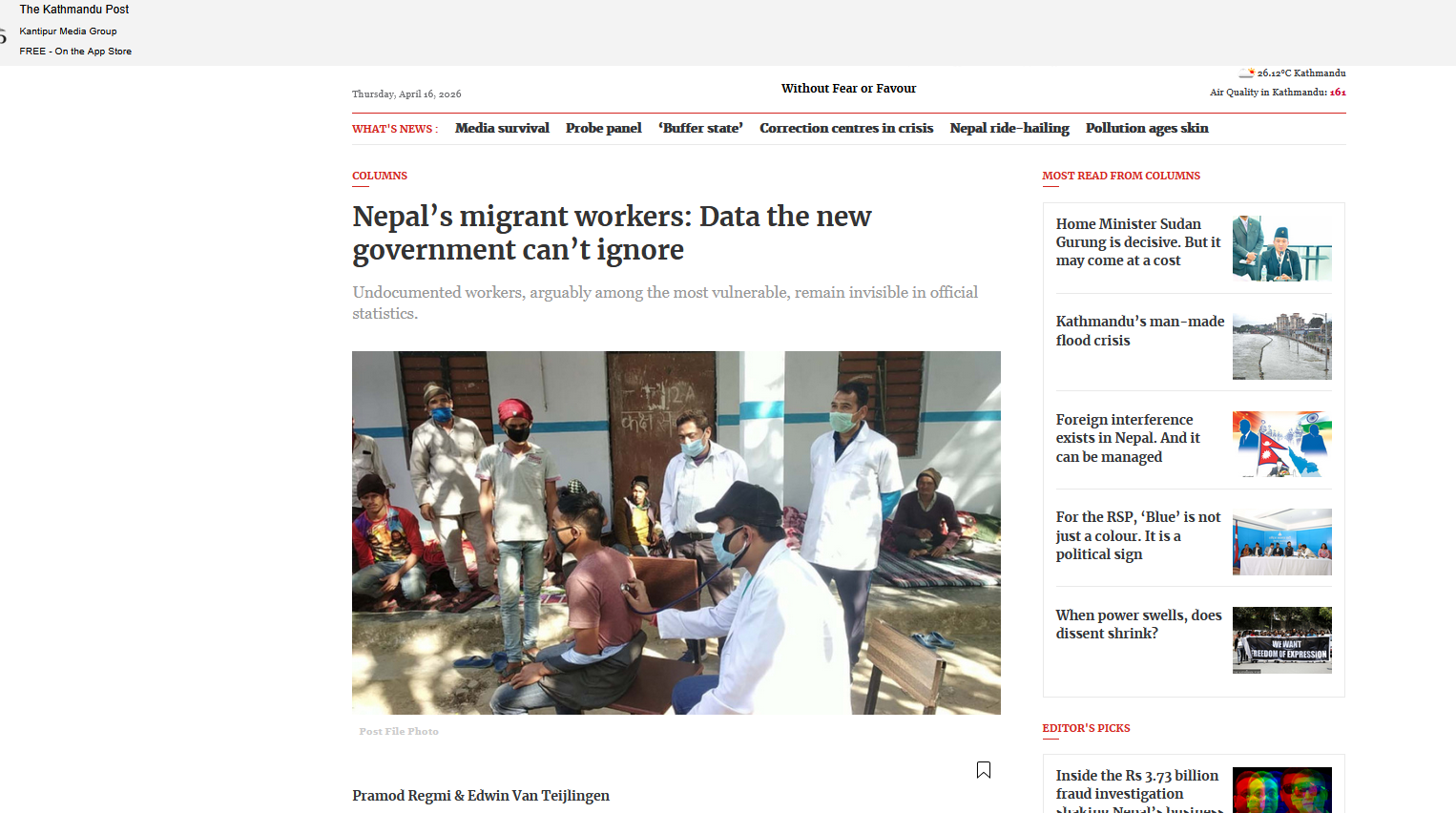
Yesterday (5th March) Dr. Pramod Regmi and Prof. Edwin van Teijlingen published a topical piece in an online newspaper in Nepal called ‘NepaliLink. This newspaper article coincided with the national elections taking place in the country. This is the first general election since Gen Z protests overturned the Government of Nepal in the autumn of 2025. Migrant labour is key to Nepal’s economy as no country in the world relies so much on workers going abroad to work and sending money home. The latter is called remittance and the total amount sent home comprises more than a quarter of the national income.
Dr. Regmi and Prof. van Teijlingen have conducted a great number of studies on the health and well-being of migrant workers from Nepal. This includes a paper ‘A comparison of chronic kidney risk among returnee Nepalese migrant workers in the countries of Gulf and Malaysia and non-migrants in Nepal: a population-based cross-sectional study’ whixh was recently accepted for publication in BMC Nephrology. With a grant from the COLT Foundation, our BU team led the first large-scale population-based interdisciplinary study examining kidney health among Nepalese migrants. Conducted in mid-2023 in one of Nepal’s highest out-migration districts, the forthcoming study compared risks between migrants and non-migrants from the same community [1]. Our study identified significantly higher rates of hypertension, diabetes, and obesity among male migrant workers compared to non-migrants. Interestingly, smoking and alcohol consumption were more common among non-migrant men. However, one in seven male migrants reported consuming potentially hazardous counterfeit or home-brewed alcohol while abroad. The findings suggest that both adverse working environments and lifestyle factors may contribute to increased heart disease among migrant workers.
Both Dr. Regmi and Prof. van Teijlingen are based in the Faculty of Health, Environment & Medical Sciences (HEMS) and in the last five years alone they have published over twenty publications about the health and well-being of migrant workers [2-21].
References
- Aryal, N., Regmi, P., Sedhain, A., Bhattarai, S., KC, R.K., Mishra, S.K., Caplin, B., Perce, N., van Teijlingen E. (2026) A comparison of chronic kidney risk among returnee Nepalese migrant workers in the countries of Gulf and Malaysia and non-migrants in Nepal: a population-based cross-sectional study, BMC Nephrology 1186/s12882-026-04872-7 (forthcoming)
-
Adhikari, Y.R., van Teijlingen, E., Regmi, P.R., Khanal, S., (2026) Parental migration for work and psychosocial problems among left-behind adolescents in Nepal, Journal of Immigrant & Minority Health (forthcoming)
-
Paudyal, P., Wasti, S.P., Neupane, P., Sapkota, J.L., Watts, C., Kulasabanathan, K., Silwal, R., Memon, A., Shukla, P, Pathak, R.S., Michelson, D., Beery, C., Moult, A., Simkhada, P., van Teijlingen, E., Cassell, J. 10, (2025) Coproducing a culturally sensitive storytelling video intervention to improve psychosocial well-being: a multimethods participatory study with Nepalese migrant workers, BMJ Open 15:e086280.
-
Regmi, P., Aryal, N., Bhattarai, S., Sedhain, A., KC, R.K., van Teijlingen, E. (2024) Exploring lifestyles, work environment and health care experience of Nepalese returnee labour migrants diagnosed with kidney-related problems. PLoS ONE 19(8): e0309203.
-
Paudyal, A.R., Harvey, O., Teijlingen, E. van, Regmi, P. R., Sharma, C. (2024). Returning Home to Nepal after Modern Slavery: Opportunities for Health Promotion. Journal of Health Promotion, 12(1), 125–132. https://doi.org/10.3126/jhp.v12i1.72713
- Regmi, P., Aryal, N., van Teijlingen, E., KC, R.K., Gautam, M. and Maharjan, S. (2024). A Qualitative Insight into Pre-Departure Orientation Training for Aspiring Nepalese Migrant Workers. Tropical Medicine and Infectious Disease, 9 (7).
-
Aryal, N., Regmi, P., Adhikari Dhakal, S., Sharma, S. and van Teijlingen, E. (2024). Moral panic, fear, stigma, and discrimination against returnee migrants and Muslim populations in Nepal: analyses of COVID-19 media content. Journal of Media Studies, 38 (2), 71-98.
-
Simkhada, P.P., van Teijlingen, E., Gurung, M., Bhujel, S., Wasti, S.P. (2024) Workplace harassment faced by female Nepalese migrants working aboard, Global Health Journal 8(3): 128-32. https://doi.org/10.1016/j.glohj.2024.08.001
- Mahato, P., Bhusal, S., Regmi, P., van Teijlingen, E. (2024). Health and Wellbeing Among Nepali Migrants: A Scoping Review. Journal of Health Promotion, 12(1): 79–90. https://doi.org/10.3126/jhp.v12i1.72699
- Regmi, P., Aryal, N., Bhattarai, S., Sedhain, A., KC, R.K. and van Teijlingen, E. (2024) Exploring lifestyles, work environment and health care experience of Nepalese returnee labour migrants diagnosed with kidney-related problems, PLoS One 19(8): e0309203. https://doi.org/10.1371/journal.pone.0309203
-
Khanal, S.P., van Teijlingen, E., Sharma, M., Acharya, J., Sharma, C., Kharel, S., Gaulee, U., Bhattarai, K., Pasa, R.B., Bohora, P. (2024) Risk Perception and Protective Health Measure Regarding COVID-19 among Nepali Labour Migrants’ Returnee from India. KMC Journal, 6(1): 313–330
- Chaudhary, M.N., Lim, V.C., Sahimin, N., Faller, E.M., Regmi, P., Aryal, N. and Azman, A.S. (2023). Assessing the knowledge of, attitudes towards, and practices in, food safety among migrant workers in Klang Valley, Malaysia. Travel Medicine and Infectious Disease, 54.
-
Gyawali, K., Simkhada, P., van Teijlingen, E.R., Manandhar, S., Silwal, R.C. (2023). Sexual Harassment Among Nepali Non-Migrating Female Partners of International Labor Migrant Men. Journal of Health Promotion, 11(1): 22–31
-
Adhikari, Y., Regmi, P., Devkota, B. and van Teijlingen, E. (2023). Forgotten health and social care needs of left-behind families of Nepali migrant workers. Journal of Health Promotion, 10, 1-4.
- Regmi, P., Dhakal Adhikari, S., Aryal, N., Wasti, S.P., van Teijlingen, E. (2022) Fear, Stigma and Othering: The Impact of COVID-19 Rumours on Returnee Migrants and Muslim Populations of Nepal, International Journal of Environmental Research & Public Health 19(15), 8986; https://doi.org/10.3390/ijerph19158986
- Regmi, P., Simkhada, P., Aryal, N., van Teijlingen, E. (2022) Excessive mortalities among migrant workers: the case of the 2022 FIFA World Cup. Europasian Journal of Medical Sciences, 4:31-32. https://doi.org/10.46405/ejms.v4i0.455
- Simkhada, P., van Teijlingen, E. and Regmi, P. (2022). Migrant Workers in Qatar: Not just an important topic during the FIFA World Cup 2022. Health Prospect: Journal of Public Health, 21 (3), 1-2.
- Aryal, N., Sedhain, A., Regmi, P.R., KC, R. K., van Teijlingen, E. (2021). Risk of kidney health among returnee Nepali migrant workers: A survey of nephrologists. Asian Journal of Medical Sciences, 12(12), 126–132. https://doi.org/10.3126/ajms.v12i12.39027
- Aryal, N., Regmi, P.R., Sedhain, A., KC, R.K., Martinez Faller, E., Rijal, A., van Teijlingen, E. (2021) Kidney health risk of migrant workers: An issue we can no longer overlook. Health Prospect 20(1):15-7
- Simkhada, B., Sah, R.K., Mercel-Sanca, A., van Teijlingen, E., Bhurtyal, Y.M. and Regmi, P. (2021). Perceptions and Experiences of Health and Social Care Utilisation of the UK-Nepali Population. Journal of Immigrant and Minority Health, 23 (2), 298-307.
Evidence Synthesis Centre open at Kathmandu University
 Last week we opened the Evidence Synthesis Centre in the School of Medical Sciences at Kathmandu University in Nepal. The centre is part of a wider initiative is funded by The British Academy and supported in the field by Green Tara Nepal. Earlier parts of this initiative included online workshop on systematic reviewing and evidence synthesis as well as face-to-face training in Nepal late last year. The project involved Bournemouth University’s Dr. Pramod Regmi and Prof. Edwin van Teijlingen both in the Faculty of Health, Environment & Medical Sciences.
Last week we opened the Evidence Synthesis Centre in the School of Medical Sciences at Kathmandu University in Nepal. The centre is part of a wider initiative is funded by The British Academy and supported in the field by Green Tara Nepal. Earlier parts of this initiative included online workshop on systematic reviewing and evidence synthesis as well as face-to-face training in Nepal late last year. The project involved Bournemouth University’s Dr. Pramod Regmi and Prof. Edwin van Teijlingen both in the Faculty of Health, Environment & Medical Sciences. 
This capacity-building project is led by Prof. Padam Simkhada from the University of Huddersfield and takes place at Kathmandu University School of Medical Sciences (KUSMS). This new Fellowship scheme is an international collaboration led by the University of Huddersfield in the UK, in close collaboration with Kathmandu University School of Medical Sciences (in Nepal), the Nepal Health Research Council, and several UK universities: Bournemouth University, the University of Sheffield, Canterbury Christ Church University, Keele University and the University of Chester. The Evidence Synthesis Centre and The British Academy grant grew out of an editorial written four years ago and published in the Journal of the Nepal Health Research Council [1]. The wider British Academy funded project on strengthening evidence synthesis for health policy-making in Nepal has been described in two recent publications [2-3].
References:
-
Simkhada, P., Dhimal, M., van Teijlingen, E., Gyanwali, P. (2022) Nepal Urgently Needs a National Evidence Synthesis Centre, Journal of Nepal Health Research Council, 20 (3): i-ii.
-
Simkhada, P., Vaidya, A., Regmi, P. P., Paudyal, P., van Teijlingen, E., Dhimal, M., Kiorala, B., Shrestha, A., Simkhada, B. (2025). Strengthening Evidence Synthesis for Health Policymaking in Nepal: A New Fellowship Initiative. Nepal Journal of Epidemiology, 15(2), 1379–1380. https://doi.org/10.3126/nje.v15i2.88516
- Vaidya, A., Simkhada, P., Silwal, R. C., Paudyal, P., Dhimal, M., Simkhada, B., van Teijlingen, E. (2025). Progress of the Unique Fellowship in Health Research Evidence Synthesis in Nepal. Nepal Journal of Epidemiology, 15(4), 1397–1398. https://doi.org/10.3126/nje.v15i4.88535
Visiting Prof. Sujan Marahatta presenting at BU
 Prof. Sujan Marahatta from Nepal will be presenting at Bournemouth University about Competency-based education of health professionals in Nepal. He will be speaking on Monday March 9th in a session jointly organised by the Centre for Midwifery & Women’s Health (CMWH) and the Centre for Wellbeing and Long-Term Health (CWLTH). The session will be in the Bournemouth Gateway Building (BGB) room 407 from 10.00 till 12.00. Prof. Marahatta is currently the Director of the Medical Education Commission in Nepal overseeing the education on the country of a wide range of health professionals including nurses and midwives. Prof. Marahatta is Visiting Professor in the Faculty of Health, Environment & Medical Sciences (FHEMS)and has been so for nearly a decade. He is also a co-author on many publications with several past and present academics in the Faculty of Health, Environment and Medical Sciences [1-20]. Former BU academics with whom Prof. Marahatta is a co-author include: Bibha Simkhada, Nirmal Aryal, Malcolm McIver, Preeti Mahato, Elaine Asbridge, Jana Kuncova, and Anneyce Knight, whilst co-authors currently based at BU include: Dr. Catherine Angell, Prof. Carol Clark, Dr. Pramod Regmi, Prof. Vanora Hundley, and Prof. Edwin van Teijlingen.
Prof. Sujan Marahatta from Nepal will be presenting at Bournemouth University about Competency-based education of health professionals in Nepal. He will be speaking on Monday March 9th in a session jointly organised by the Centre for Midwifery & Women’s Health (CMWH) and the Centre for Wellbeing and Long-Term Health (CWLTH). The session will be in the Bournemouth Gateway Building (BGB) room 407 from 10.00 till 12.00. Prof. Marahatta is currently the Director of the Medical Education Commission in Nepal overseeing the education on the country of a wide range of health professionals including nurses and midwives. Prof. Marahatta is Visiting Professor in the Faculty of Health, Environment & Medical Sciences (FHEMS)and has been so for nearly a decade. He is also a co-author on many publications with several past and present academics in the Faculty of Health, Environment and Medical Sciences [1-20]. Former BU academics with whom Prof. Marahatta is a co-author include: Bibha Simkhada, Nirmal Aryal, Malcolm McIver, Preeti Mahato, Elaine Asbridge, Jana Kuncova, and Anneyce Knight, whilst co-authors currently based at BU include: Dr. Catherine Angell, Prof. Carol Clark, Dr. Pramod Regmi, Prof. Vanora Hundley, and Prof. Edwin van Teijlingen.

References:
- Simkhada P, van Teijlingen E, Marahatta SB. Mental health services in Nepal: Is it too late? Journal of Manmohan Memorial Institute of Health Sciences 2015:1(4):1-2.
- Simkhada P, van Teijlingen E, Winter RC, Fanning C, Dhungel A, Marahatta SB. Why are so many Nepali women killing themselves? A review of Key issues. Journal of Manmohan Memorial Institute of Health Sciences 2015:1(4):43-49.
- Simkhada B, Mackay S, Khatri R, Sharma CK., Pokhrel T, Marahatta SB., Angell C, van Teijlingen E, Simkhada P. (2016) Continual Professional Development (CPD): Improving Health Prospect15 (3):1-3.
- Regmi PR, Simkhada P, van Teijlingen E, Pant PR, Kurmi O, Marahatta SB. What can we learn from the Nepal Health Facility Survey 2015? JMMIHS 2017;3 (1):1-5.
- van Teijlingen E, Marahatta SB, Simkhada P, McIver M, Sharma JS. Developing an international higher education partnership between high and low-income countries: two case studies.
- Journal of Manmohan Memorial Institute of Health Sciences 2017;3 (1):94-100.
- Simkhada P, van Teijlingen E, Simkhada, B, Regmi P, Aryal N, Marahatta SB. Experts warn Nepal government not to reduce local public health spending. Journal of Manmohan Memorial Institute of Health Sciences. 2018;4(1):1-3.
- Regmi PR, van Teijlingen E, Neupane SR, Marahatta SB. Hormone use among Nepali transgender women: a qualitative study. BMJ Open 2019;9:e030464. doi:10.1136/ bmjopen-2019-030464
- Adhikarya, P., Balen, J., Gautam, S., Ghimire, S., Karki, J., Lee, A., Marahatta, SB., Panday, S., Pohl, G., Rushton, S., Sapkota, S., Simkhada, P.P., Subedi, M., van Teijlingen, E., & the Nepal Federal Health System team (2020) The COVID-19 pandemic in Nepal: Emerging evidence on the effectiveness of action by, and cooperation between, different levels of government in a federal system, Journal of Karnali Academy of Health Sciences 2020;3;3-9.
- Sathian, B., Asim, M., Mekkodathil, A., van Teijlingen, E., Subramanya, S.H., Simkhada, P., Marahatta, S.B., Shrestha, U.M. (2020) Impact of COVID-19 on community health: A systematic review of a population of 82 million, Journal of Advanced Internal Medicine 2020; 9(1): 4-11. https://www.nepjol.info/index.php/JAIM/article/view/29159
- Khatri, RJ, van Teijlingen, E, Marahatta, SB, Simkhada, P, Mackay, S and Simkhada, B. Exploring the Challenges and Opportunities for Continuing Professional Development for Nurses: A Qualitative Study with Senior Nurse Leaders in Nepal. Journal of Manmohan Memorial Institute of Health Sciences. 2021 7(1):15-29.
- Sapkota S, Panday S, Wasti, S.P., Lee, A., Balen, J., van Teijlingen, E., Rushton, S., Subedi, M., Gautam, S., Karki., J., Adhikary, P., Marahatta SB et al.,Health System Strengthening: The Role of Public Health in Federal Nepal JNEPHA. 2022;7(1):36-42.
- van Teijlingen, E., Thapa, D., Marahatta, S.B., Sapkota, J.L., Regmi, P. Sathian, B. (2022) Editors and Reviewers: Roles and Responsibilities, In: Wasti, S.P., et al. (Eds.) Academic Writing and Publishing in Health & Social Sciences, Kathmandu, Nepal: Himal Books: 32-37.
- Mahato P, Adhikari B, Marahatta SB, et al. (2023) Perceptions around COVID-19 and vaccine hesitancy: A qualitative study in Kaski district, Western Nepal. PLOS Glob Public Health 3(2): e0000564. https://doi.org/10.1371/journal.pgph.0000564
- Marahatta SB, Regmi P, Knight A, Kuncova J, Asbridge E, Khanal DP, van Teijlingen E. Staff-student exchange between MMIHS and Bournemouth University. Journal of Manmohan Memorial Institute of Health Sciences. 2023;8(1)1-5
- Sapkota S, Dhakal A, Rushton S, van Teijlingen E, Marahatta SB, Lee ACK, Balen J. The impact of decentralisation on health systems: a systematic review of reviews. BMJ Global Health 2023;8:e013317. doi:10.1136/ bmjgh-2023-013317
- Sapkota, S, Rushton S, van Teijlingen E. Marahatta SB et al. Participatory policy analysis in health policy and systems research: reflections from a study in Nepal. Health Research Policy & Systems 22, 7 (2024). https://doi.org/10.1186/s12961-023-01092-5
- Wasti SP, van Teijlingen E, Simkhada P, Rushton S, Balen J, Subedi M, Marahatta SB et al. Selection of study sites and participants for research into Nepal’s federal health system. WHO South-East Asia J Public Health 2023;12:116-9.
- Clark CJ, Marahatta SB, Hundley VA. The prevalence of pain catastrophising in nulliparous women in Nepal; the importance for childbirth. PLoS ONE 2024;19(8): e0308129. https://doi. org/10.1371/journal.pone.0308129.
- Sapkota, S., Rushton, S., van Teijlingen, E., Subedi, M., Balen, J., Gautam, S., Adhikary, P., Simkhada, P., Wasti, SP., Karki, JK., Panday, S., Karki, A., Rijal, B., Joshi, S., Basnet, S., Marahatta, SB. (2024) Participatory policy analysis in health policy and systems research: reflections from a study in Nepal. Health Research & Policy Systems, 22(7) https://doi.org/10.1186/s12961-023-01092-5 .
Nursing Research REF Impact in Nepal
The Nepal Nursing Council has made Continuing Professional Development (CPD) compulsory for all nurses and midwives wanting to re-enrol from tomorrow. Starting on 15th January 2025 all nurses and midwives who want to re-register will have to show evidence of having conducted recent training to maintain and enhance their knowledge, skills, and professional competence. According to the new provision, licences will not be renewed unless applicants have completed a minimum of 60 hours of training within the preceding six years. This change in regulation is largely driven by research driven by two UK universities, and BU is one of them.
As early as 2016 the research team called for a move to a system of post-registration with compulsory further learning and regular updating of skills, adding that “the introduction of CPD will be beneficial to all nurses in Nepal” [1]. The key argument was that If Nepal does not establish CPD requirements, only some staff will engage with training activities, it will be ad hoc driven by personal interests rather than service needs. An even greater concern was that staff will seek only the free training made available by either the government and/or INGOs (International Non-Governmental Organisations) rather than CPD most relevant to their current practices.
 To generate the evidence that CPD is vital in Nepal, the team led by Dr. Bibha Simkhada conducted interviews with nurse leader in the country to understand perspectives on existing on-the-job training and Continuous Professional Development more generally [2]. Bibha, currently Reader in Nursing at the University of Huddersfield, worked at Bournemouth University for several years during this research. Next, the researchers conducted focus group discussions with other relevant stakeholders [3]. These research findings were disseminated to stakeholders in Kathmandu, including the NNC (Nepal Nursing Council), MIDSON (Midwifery Society of Nepal), NAN (Nursing Association of Nepal), and the Ministry of Health & Population as well as to a wider audience through a call under the heading ‘Nepal needs Continuing Professional Development for Re-registration in Nursing and Midwifery’ [4].
To generate the evidence that CPD is vital in Nepal, the team led by Dr. Bibha Simkhada conducted interviews with nurse leader in the country to understand perspectives on existing on-the-job training and Continuous Professional Development more generally [2]. Bibha, currently Reader in Nursing at the University of Huddersfield, worked at Bournemouth University for several years during this research. Next, the researchers conducted focus group discussions with other relevant stakeholders [3]. These research findings were disseminated to stakeholders in Kathmandu, including the NNC (Nepal Nursing Council), MIDSON (Midwifery Society of Nepal), NAN (Nursing Association of Nepal), and the Ministry of Health & Population as well as to a wider audience through a call under the heading ‘Nepal needs Continuing Professional Development for Re-registration in Nursing and Midwifery’ [4].
These papers all argue that promoting CPD benefits the quality of health care. Indirectly, it builds confidence in the general population as it is guarantee to the individual patient in Nepal that the nurses and midwives, who are treating them, have up-to-date skills and knowledge. In addition, it strengthens the NNC as it supports to professionalise nursing and midwifery in Nepal and bring the standard of nursing and midwifery practices to a higher and internationally comparable level.
The research work at BU was supported by small amounts of QR funding through BU Centre for Excellence in Learning (CEL) in 2016, the Centre for Midwifery & Women’s Health in 2018 and the Faculty of Health & Social Sciences in 2019. This shows that well-designed research conducted by researchers who have insight into the political landscape of health services in Nepal can have a great impact with minimal resources.
Prof. Edwin van Teijlingen (BU REF lead UoA3)
&
Dr. Vikram Mohan (UoA3 REF Impact Champion)
References
- Simkhada, B, Mackay, S, Khatri, R., Sharma, C.K., Pokhrel, T, Marahatta, S, Angell, C, van Teijlingen, E., Simkhada, P (2016) Continual Professional Development (CPD): Improving Quality of Nursing Care in Nepal Health Prospect 15 (3):1-3.
- Khatri R, van Teijlingen E, Marahatta SB, Simkhada P, Mackay S, Simkhada B (2021) Exploring the Challenges and Opportunities for Continuing Professional Development for Nurses: A Qualitative Study with Senior Nurse Leaders in Nepal Journal of Manmohan Memorial Institute of Health Sciences. 7(1), 15-29.
- Simkhada B, van Teijlingen E, Pandey A, Sharma CK, Simkhada P, Singh DR (2023) Stakeholders’ Perceptions of Continuing Professional Development among Nepalese Nurses: A Focus Group Study Nursing Open.10(5).
- Simkhada B, van Teijlingen E, Sharma C, Pandey A, Simkhada P. (2023) Nepal needs Continuing Professional Development for Re-registration in Nursing and Midwifery Journal of Nepal Health Research Council, 21(60):541-42.
Final Bournemouth University publication of 2025
Happy New Year and we hope it will be prosperous and healthy.  On the last day of 2025 the Nepal Journal of Epidemiology published our editorial ‘Progress of the Unique Fellowship in Health Research Evidence Synthesis in Nepal‘ [1]. Co-authors of this editorial include Faculty of Health & Social Sciences Visiting Faculty: Prof. Padam Simkhada and Dr. Bibha Simkhada who are both grant holders on the British Academy grant which also includes BU’s Dr. Pramod Regmi. The journal editor added a photo of our recent three-day event on research capacity building in Dhulikhel (Nepal) to the cover of the December issue.
On the last day of 2025 the Nepal Journal of Epidemiology published our editorial ‘Progress of the Unique Fellowship in Health Research Evidence Synthesis in Nepal‘ [1]. Co-authors of this editorial include Faculty of Health & Social Sciences Visiting Faculty: Prof. Padam Simkhada and Dr. Bibha Simkhada who are both grant holders on the British Academy grant which also includes BU’s Dr. Pramod Regmi. The journal editor added a photo of our recent three-day event on research capacity building in Dhulikhel (Nepal) to the cover of the December issue. Nepalese researchers, academics, policymakers and practitioners are undertaking a unique Fellowship in evidence synthesis and evidence-based policy making. This Fellowship is part of a larger project called ‘Evidence Informed Health Policy Making in Nepal (EHPN)’, funded by the British Academy. After our training event Dr. Regmi had the opportunity to present our (2022) textbook Academic Writing and Publishing in Health and Social Sciences to His Excellency Mr. Madhav Chaulagain, Nepal’s newly appointed Minister of Forest & Environment.
Nepalese researchers, academics, policymakers and practitioners are undertaking a unique Fellowship in evidence synthesis and evidence-based policy making. This Fellowship is part of a larger project called ‘Evidence Informed Health Policy Making in Nepal (EHPN)’, funded by the British Academy. After our training event Dr. Regmi had the opportunity to present our (2022) textbook Academic Writing and Publishing in Health and Social Sciences to His Excellency Mr. Madhav Chaulagain, Nepal’s newly appointed Minister of Forest & Environment.
Evidence-informed policy making developed out of the earlier idea of ‘evidence-based policy making’. The central idea behind evidence-based policy making was that it should be largely (or even solely) guided by evidence. Evidence-informed policy making adds that policies should not just be evidence-based they should also be feasible, appropriate for their context and aligned with stakeholders’ values and therefore one would expect meaningful input from these stakeholders. This is the second editorial highlighting our research capacity-building work in Nepal. The first editorial ‘Strengthening Evidence Synthesis for Health Policymaking in Nepal: A New Fellowship Initiative’ appeared in an earlier edition of the Nepal Journal of Epidemiology [2].

Prof. Edwin van Teijlingen
Centre for Midwifery & Women’s Health

References:
- Vaidya, A., Simkhada, P., Silwal, R. C., Paudyal, P., Dhimal, M., Simkhada, B., van Teijlingen, E. (2025). Progress of the Unique Fellowship in Health Research Evidence Synthesis in Nepal. Nepal Journal of Epidemiology, 15(4), 1397–1398.
- Simkhada, P., Vaidya, A., Regmi, P. P., Paudyal, P., van Teijlingen, E., Dhimal, M., Shrestha, A., Koirala, B., Simkhada, B. (2025). Strengthening Evidence Synthesis for Health Policymaking in Nepal: A New Fellowship Initiative. Nepal Journal of Epidemiology, 15(2), 1379–1380.
New Nepal scoping review on maternal & neonatal health
Today, Discover Public Health, published our latest academic paper on maternity and neonatal care in Nepal [1]. Our latest paper ‘A scoping review of interventions to improve maternal and neonatal care in Nepal‘ is lead by Dr. Sharada Prasad Wasti at the University of Greenwich and co-authored by Bournemouth University’s Prof. Edwin van Teijlingen. 
For this scoping review we found 418 studies, and twenty were included, which used various interventions that aimed to improve maternal and neonatal health. Five overarching interventions were identified: (1) community-based maternal health literacy; (2) health facility strengthening, including health staff training, (3) mobilisation of female community health volunteers (FCHV) for birth preparedness and identifying danger signs; (4) mobile health messaging, and (5) involving husbands in improving the uptake of maternal and neonatal care. Most interventions were a mixture of activities with a combination of interventions rather than a single intervention.
The authors note that no single intervention is sufficient on its own; indeed, a combination of approaches is needed to improve the uptake of maternal and neonatal care services.
This scientific paper in Discover Public Health is open access and, therefore, freely available worldwide to anybody with internet access. Interestingly, the journal has added an AI generated summary, despite the fact that we as authors had provided a perfectly useful abstract.

Reference:
- Wasti, S.P., van Teijlingen, E., Adhikari, N. Morgan, J. (2025) A scoping review of interventions to improve maternal and neonatal care in Nepal. Discover Public Health 22, 855 . https://doi.org/10.1186/s12982-025-01241-x
British Academy funded capacity-building training in Nepal
 Yesterday we reached third day of the three-day Fellowship training workshop in Dhulikhel, Nepal on evidence synthesis. This capacity-building project is led by the University of Huddersfield and takes place at Kathmandu University School of Medical Sciences (KUSMS). This new Fellowship scheme is an international collaboration led by the University of Huddersfield in the UK, in close collaboration with Kathmandu University School of Medical Sciences (in Nepal), the Nepal Health Research Council, and several UK universities: Bournemouth University, the University of Sheffield, Canterbury Christ Church University, Keele University and the University of Chester. This unique Fellowship started online in the autumn of 2025 and is part of a larger project on strengthening institutional knowledge and capacity of federal, provincial and local governments for evidence-informed health policymaking in Nepal. This important initiative is funded by The British Academy and supported in the field by Green Tara Nepal [1]. The project involved Bournemouth University’s Dr. Pramod Regmi and Prof. Edwin van Teijlingen both in the Faculty of Health, Environment & Medical Sciences.
Yesterday we reached third day of the three-day Fellowship training workshop in Dhulikhel, Nepal on evidence synthesis. This capacity-building project is led by the University of Huddersfield and takes place at Kathmandu University School of Medical Sciences (KUSMS). This new Fellowship scheme is an international collaboration led by the University of Huddersfield in the UK, in close collaboration with Kathmandu University School of Medical Sciences (in Nepal), the Nepal Health Research Council, and several UK universities: Bournemouth University, the University of Sheffield, Canterbury Christ Church University, Keele University and the University of Chester. This unique Fellowship started online in the autumn of 2025 and is part of a larger project on strengthening institutional knowledge and capacity of federal, provincial and local governments for evidence-informed health policymaking in Nepal. This important initiative is funded by The British Academy and supported in the field by Green Tara Nepal [1]. The project involved Bournemouth University’s Dr. Pramod Regmi and Prof. Edwin van Teijlingen both in the Faculty of Health, Environment & Medical Sciences.
Some 28 Fellows have been selected from nearly one hundred applicants to help build capacity in the field of evidence synthesis with overall aim to promote evidence-informed policymaking in Nepal. This is longstanding aim of the researcher as highlighted in previous call for an evidence-based policy centre in Nepal [2].
1. Simkhada P, Vaidyal A, Regmi P, Paudyal P, van Teijlingen E, Dhimal M, Koirala B, Shresthe A, Simkhada B (2025) Strengthening Evidence Synthesis for Health Policymaking in Nepal: A New Fellowship Initiative, Nepal Journal of Epidemiology, 15(2), 1379–1380. https://doi.org/10.3126/nje.v15i2.88516
2. Simkhada P, Dhimal M, van Teijlingen E, Gyanwali P (2022). Nepal Urgently Needs a National Evidence Synthesis Centre, Nepal Journal of Epidemiology, 20 (3): i-ii.
BU academic publishes in online newspaper in Nepal
 Last week the internet newspaper Online Khabar published ‘Celebrating Nepal Female Community Health Volunteers, but for how much longer?‘. This article is written by Sankalpa Bhattarai, a researcher based at Green Tara Nepal, and BU’s Prof. Edwin van Teijlingen about the future of Female Community Health Volunteers (FCHVs) in Nepal. In the late 1980s the Government of Nepal introduced the FCHV programmea at a time, Nepal was one of only two countries in the world where the life expectancy for women was lower than that of men. These FCHVs were recruited locally in their own communities to help reduce infant and maternal mortality. They provided health education, immunisation, and information on family planning and hygiene, as well as offering basic first aid services and referring people in their communities to basic or advanced health services when needed.
Last week the internet newspaper Online Khabar published ‘Celebrating Nepal Female Community Health Volunteers, but for how much longer?‘. This article is written by Sankalpa Bhattarai, a researcher based at Green Tara Nepal, and BU’s Prof. Edwin van Teijlingen about the future of Female Community Health Volunteers (FCHVs) in Nepal. In the late 1980s the Government of Nepal introduced the FCHV programmea at a time, Nepal was one of only two countries in the world where the life expectancy for women was lower than that of men. These FCHVs were recruited locally in their own communities to help reduce infant and maternal mortality. They provided health education, immunisation, and information on family planning and hygiene, as well as offering basic first aid services and referring people in their communities to basic or advanced health services when needed.
 The FCHV programme is one of the most successful parts of the country’s health system, and recognised worldwide for offering basic care in a system of harmony between local volunteers and the communites they live in, as such meaningful connections can have a profound impact on people’s well-being. There are FCHVs in most villages and the volunteer workforce comprises over fifty thousand women spread across the country. Th future of this FCHV programme is currently being discussed with four possible strategies emerging: (1) redefining FCHV roles; (2) modernization and skills upgrade; (3) establishing permanent support and incentives; and (4) formalizing their role in crisis response.
The FCHV programme is one of the most successful parts of the country’s health system, and recognised worldwide for offering basic care in a system of harmony between local volunteers and the communites they live in, as such meaningful connections can have a profound impact on people’s well-being. There are FCHVs in most villages and the volunteer workforce comprises over fifty thousand women spread across the country. Th future of this FCHV programme is currently being discussed with four possible strategies emerging: (1) redefining FCHV roles; (2) modernization and skills upgrade; (3) establishing permanent support and incentives; and (4) formalizing their role in crisis response. 
The online newspaper article is based on a paper we published last year as a Commentary in the Journal of Manmohan Memorial Institute of Health Sciences [1]. Our previous research work on FCHVs included a paper in PLOS Global Public Health [2], as well as two further papers based on the Ph.D. study by Dr. Sarita Panday [3-4].
We like to take this opportunity to thank Dr. Pramod Regmi, Principal Academic in International Health in the Faculty of Health, Environment & Medical Science, for connecting us to the editor of Online Khabal.
Prof. Edwin van Teijlingen
Centre for Midwifery & Women’s Health
References
- Bhattarai, S., & van Teijlingen, E. (2024). Nepal Needs A Two-Pronged Approach to Secure Future of Its Female Community Health Volunteers (FCHVs). Journal of Manmohan Memorial Institute of Health Sciences, 9(1), 43–48. https://doi.org/10.3126/jmmihs.v9i1.68640
- Panday, S., Barnes, A., van Teijlingen, E. (2024) Exploring the motivations of female community health volunteers in primary healthcare provision in rural Nepal: a qualitative study, PLOS Global Public Health Aug 1;4(8):e0003428. doi: 10.1371/journal.pgph.0003428.
- Panday, S., Bissell, P., van Teijlingen, E., Simkhada, P. (2017) The contribution of female community health volunteers (FCHVs) to maternity care in Nepal: a qualitative study, BMC Health Services Research 17:623 be/vz9C
- Panday, S., Bissell, P., van Teijlingen, E., Simkhada, P. (2019) Perceived barriers to accessing female community health volunteers’ services amongst ethnic minority women in Nepal: a qualitative study, PLoS ONE 14(6): e0217070 https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0217070
New PhD publication on Nepal’s migrant workers
 Congratulations to BU postgraduate student Yagya Adhikari, who has just been informed by the editor of the Journal of Immigrant & Minority Health that his paper “Parental migration for work and psychosocial problems among left-behind adolescents in Nepal” [1] has been accepted for publication. Yagya’s PhD is based in the Faculty of Health, Environment & Medical Science. He is supervised by Dr. Pramod Regmi and Prof. Edwin van Teijlingen with support from Mr. Sudip Khanal, Lecturer in Biostatistics, at Manmohan Memorial Institute of Health Sciences (MMIHS) in Kathmandu. This is the second paper from Yagya’s PhD the first one was published at the start of his PhD studies [2]. Both papers are published in Open Access journals and therefor will be freely available to read by anyone in the world with internet access.
Congratulations to BU postgraduate student Yagya Adhikari, who has just been informed by the editor of the Journal of Immigrant & Minority Health that his paper “Parental migration for work and psychosocial problems among left-behind adolescents in Nepal” [1] has been accepted for publication. Yagya’s PhD is based in the Faculty of Health, Environment & Medical Science. He is supervised by Dr. Pramod Regmi and Prof. Edwin van Teijlingen with support from Mr. Sudip Khanal, Lecturer in Biostatistics, at Manmohan Memorial Institute of Health Sciences (MMIHS) in Kathmandu. This is the second paper from Yagya’s PhD the first one was published at the start of his PhD studies [2]. Both papers are published in Open Access journals and therefor will be freely available to read by anyone in the world with internet access.

References:
- Adhikari, Y.R., van Teijlingen, E., Regmi, P.R., Khanal, S., Parental migration for work and psychosocial problems among left-behind adolescents in Nepal, Journal of Immigrant & Minority Health (forthcoming)
- Adhikari, Y.R., Regmi, P.R., Devkota, B., van Teijlingen, E.R. (2022) Forgotten health and social care needs of left-behind families of Nepali migrant workers. Journal of Health Promotion, 10(1):1–4. https://doi.org/10.3126/jhp.v10i1.50976
New Centre for Midwifery & Women’s Health (CMHW) paper on Nepal
Last week the international Journal of Water, Sanitation and Hygiene for Development emailed to tell that our paper ‘Exploring handwashing knowledge and practice among lactating mothers in Kathmandu’s slum communities’ [1] had been accepted for publication.
It is widely known that poor access to good quality water, sanitation, and hygiene (WASH) lead to high morbidity in young children. The paper reports on a cross-sectional study conducted with 127 breastfeeding mothers in two slum settlements in Nepal’s capital. It found that most had a good knowledge of WASH and appropriate washing of hands. However, the prevalence of illness among children whose mothers had only basic education was 26% higher than those whose mothers had completed secondary education. Family income and hand-washing practice were also significantly associated with child health (p < 0.01). Nearly three in four (73.2%) of children had experienced health issues, particularly diarrhoea, in the past half year.
The authors concluded that strengthening maternal hand-hygiene education programmes, particularly for lactating mothers, and improving WASH infrastructure are necessary, as well as promoting affordable hand-washing solutions in urban slums.
Prof. Edwin van Teijlingen

Reference:
- Devkota, G.P., Sharma, M.K., Sherpa, S., Khanal, T.R., Devkota, B., van Teijlingen, E. (2025) Exploring handwashing knowledge and practice among lactating mothers in Kathmandu’s slum communities, Nepal, Journal of Water, Sanitation and Hygiene for Development, 15:1-10. doi: 10.2166/washdev.2025.084
Nepal migrant workers returning from India
Nepal has been in the world news this week for the wrong reasons, with young protesters burning down the parliament, and damaging many government building in all seven provinces. Some 30 young people died in the process and and thousands of sometimes dangerous prisoners were freed. After the political and social upheaval in the country this past week, Nepalese migrant workers are beginning to return home from India to be with their families. Today (Friday 12th September) the BBC online reported under the heading ‘Worried migrants head home from India after Nepal turmoil‘.
The journalist interviewed both migrant workers and students from Nepal living in India. The piece also cited several studies on Nepalese migrant workers in India, including a Bournemouth University (BU) study with the title ‘The Health of Nepali Migrants in India: A Qualitative Study of Lifestyles and Risks‘ [1]. This publication is one of the many published papers on the health and well-being of Nepalese migrant workers conducted in BU’s Faculty of Health, Environment & Medical Sciences. The lead author of this paper in theInternational Journal of Environmental Research and Public Health is Dr. Pramod Regmi, Principal Academic in International Health. 
References:
- Regmi PR, van Teijlingen E, Mahato P, Aryal N, Jadhav N, Simkhada P, Zahiruddin QS, Gaidhane A. (2019) The Health of Nepali Migrants in India: A Qualitative Study of Lifestyles and Risks. Int J Environ Res Public Health. 16(19):3655. doi: 10.3390/ijerph16193655.
UK Turing Scheme: My student mobility programme in Nepal
 My name is Anjana Regmi Paudyal, and I am a PhD student in the Faculty of Health, Environment and Medical Sciences (HEMS), Bournemouth University (BU). My doctoral research focuses on modern slavery, particularly the opportunities and barriers to survivors reintegrating into their families and communities. I was honoured to take part in the Turing Scheme traineeship and other international academic activities in Nepal, which became a truly transformative experience both personally and professionally. The Turing Scheme lasted four weeks and was hosted by the Manmohan Memorial Institute of Health Sciences (MMIHS) in Kathmandu.
My name is Anjana Regmi Paudyal, and I am a PhD student in the Faculty of Health, Environment and Medical Sciences (HEMS), Bournemouth University (BU). My doctoral research focuses on modern slavery, particularly the opportunities and barriers to survivors reintegrating into their families and communities. I was honoured to take part in the Turing Scheme traineeship and other international academic activities in Nepal, which became a truly transformative experience both personally and professionally. The Turing Scheme lasted four weeks and was hosted by the Manmohan Memorial Institute of Health Sciences (MMIHS) in Kathmandu.
 My traineeship was arranged through Bournemouth University in partnership with MMIHS in Kathmanduand it was supported by my BU supervisors Dr. Orlanda Harvey and Prof. Edwin van Teijlingen. I chose this placement because MMIHS has a strong research culture and offers opportunities to collaborate with students, faculty, and NGOs working in migration and modern slavery.
My traineeship was arranged through Bournemouth University in partnership with MMIHS in Kathmanduand it was supported by my BU supervisors Dr. Orlanda Harvey and Prof. Edwin van Teijlingen. I chose this placement because MMIHS has a strong research culture and offers opportunities to collaborate with students, faculty, and NGOs working in migration and modern slavery.
From the very beginning, I felt warmly welcomed by academics and students, which helped me settle in quickly. The first week was spent getting to know the university, its values, and its research culture. I particularly enjoyed informal discussions with first- and second-year MSc students, where we shared ideas and experiences across different academic settings.
By the second week, the focus shifted towards intensive academic engagement. I participated in a  research workshop on grant applications, systematic reviews, and qualitative research methods led by expert guest speakers. These sessions sharpened my skills in data analysis and literature reviews, giving me fresh insights into areas highly relevant to my own PhD. Alongside this, I began engaging with NGOs (Non-Governmental Organisations) working in the field of migration and modern slavery. I met with Ms. Manju Gurung, Director of POURAKHI Nepal, an organisation that supports female returnee migrants and survivors of trafficking. I also gathered policy documents and insights from Green Tara Nepal (GTN) and the Nepal Development Society (NeDS), both of which have significant experience in migration health. These connections will help to shape my upcoming PhD fieldwork.
research workshop on grant applications, systematic reviews, and qualitative research methods led by expert guest speakers. These sessions sharpened my skills in data analysis and literature reviews, giving me fresh insights into areas highly relevant to my own PhD. Alongside this, I began engaging with NGOs (Non-Governmental Organisations) working in the field of migration and modern slavery. I met with Ms. Manju Gurung, Director of POURAKHI Nepal, an organisation that supports female returnee migrants and survivors of trafficking. I also gathered policy documents and insights from Green Tara Nepal (GTN) and the Nepal Development Society (NeDS), both of which have significant experience in migration health. These connections will help to shape my upcoming PhD fieldwork.
During the third week, it was my turn to share. I presented my PhD project, and my approach, using photo elicitation, is relatively new in Nepalese research, therefore, it sparked great curiosity among students and faculty. The discussions that followed were highly rewarding, especially around ethical considerations and practical challenges. I was struck by the students’ engagement, particularly the second-year MSc cohort, who found the sessions useful for their own research journeys.
As my time in Nepal came to an end, I reflected on the differences between teaching and learning styles in the UK and Nepal. I spoke with students about the UK system, where independent study and varied assessment methods are emphasised, which was particularly valuable for those considering postgraduate studies abroad. Beyond academia, I was fortunate to experience cultural festivals within and beyond Kathmandu Valley, which deepened my appreciation of Nepal’s vibrant traditions and community spirit.
 I was fortunate to witness the “Gaijatra Festival” in Bhaktapur, Nepal. Gai Jatra is a Newari Hindu festival that honours deceased loved ones by parading decorated cows or children dressed as cows through the streets. The belief is that cows guide souls to the afterlife. Celebrated around the August full moon, the festival features music, dance, humor, and satire to provide comfort to grieving families and encourage them to embrace life despite their loss.
I was fortunate to witness the “Gaijatra Festival” in Bhaktapur, Nepal. Gai Jatra is a Newari Hindu festival that honours deceased loved ones by parading decorated cows or children dressed as cows through the streets. The belief is that cows guide souls to the afterlife. Celebrated around the August full moon, the festival features music, dance, humor, and satire to provide comfort to grieving families and encourage them to embrace life despite their loss.
Looking back, this traineeship not only enhanced my academic and research skills but also strengthened my confidence in working across cultures and linking theory with practice. It confirmed my motivation to pursue a global research career and taught me the importance of being open, flexible, and curious. My greatest achievement was being able to present and discuss my methodology with such an engaged audience, while also building long-term connections with NGOs and academic partners.
I would wholeheartedly recommend the Turing Scheme to other students. It is challenging but deeply rewarding, offering the chance to grow personally, academically, and professionally while contributing meaningfully to international collaborations. The environment at MMIHS was  welcoming, though more structured compared to the UK. Students showed huge interest in UK teaching and assessment styles. Most academic sessions were in English, but some conversations were in Nepali, which helped me practice my language skills and build rapport.
welcoming, though more structured compared to the UK. Students showed huge interest in UK teaching and assessment styles. Most academic sessions were in English, but some conversations were in Nepali, which helped me practice my language skills and build rapport.
If you get the opportunity: Say yes to goin abroad on the Turing Scheme. It challenges you, but the growth and insights are worth it. I am much more confident working with diverse groups, whether in academic or NGO settings. Presenting my PhD methodology in Nepal and receiving recognition and engagement from students and academics. Academic presentation, intercultural dialogue, trauma-informed sensitivity, networking with NGOs, and collaborative learning. Absolutely. The Turing Scheme was transformative for both my personal and professional development.
Conducting training in Kathmandu by BU academic
This week Dr. Pramod Regmi, who is Principal Academic in International Health in the Faculty of Health & Social Sciences, taught a CPD refresher workshop on systematic reviewing in Kathmandu. This workshop is part of our long-standing Memorandum of Agreement between Bournemouth University (BU) and Manmohan Memorial Institute of Health Sciences (MMIHS) in Nepal. The teaching aimed to refresh knowledge and provide practical training on various aspects of the systematic review process, including literature searching, study selection, data extraction, critical appraisal, and synthesis. The programme, which included both staff and Master students, was jointly organized by MMIHS and BU.

The staff at MMIHS also welcome BU’s Ph.D. student Ms. Anjana Paudyal. Anjana is currently in Nepal as part of the UK’s Turing Scheme Traineeship Programme. Over the past few years MMIHS have kindly hosted several BU students who came to Nepal under the Turing Scheme. Anjana’s Ph.D. focuses on human trafficking, which is form of modern slavery. Despite being a global problem, modern slavery is understudied and poorly understood. Victims of modern slavery are exploited and can experience significant physical, psychological, or sexual, and reproductive health problems. Until recently, there has been little research in this field, especially in low-income countries such as Nepal. Anjana”s Ph.D. fits in with BU’s collaboration with the US-based La Isla Network, the Johns Hopkins University Bloomberg School of Public Health and the Nepal Development Society (for details click here!). Led by La Isla Network, we are leading the first-ever international effort to research and address trafficking among Nepalese labour migrants. The work is funded by a $4 million cooperative agreement awarded by the U.S. Department of State’s Office to Monitor and Combat Trafficking in Persons, International Programs.
Until recently, there has been little research in this field, especially in low-income countries such as Nepal. Anjana”s Ph.D. fits in with BU’s collaboration with the US-based La Isla Network, the Johns Hopkins University Bloomberg School of Public Health and the Nepal Development Society (for details click here!). Led by La Isla Network, we are leading the first-ever international effort to research and address trafficking among Nepalese labour migrants. The work is funded by a $4 million cooperative agreement awarded by the U.S. Department of State’s Office to Monitor and Combat Trafficking in Persons, International Programs.

Prof. Edwin van Teijlingen
Centre for Midwifery & Women’s Health
BU attendance at third annual GCPHR meeting in June
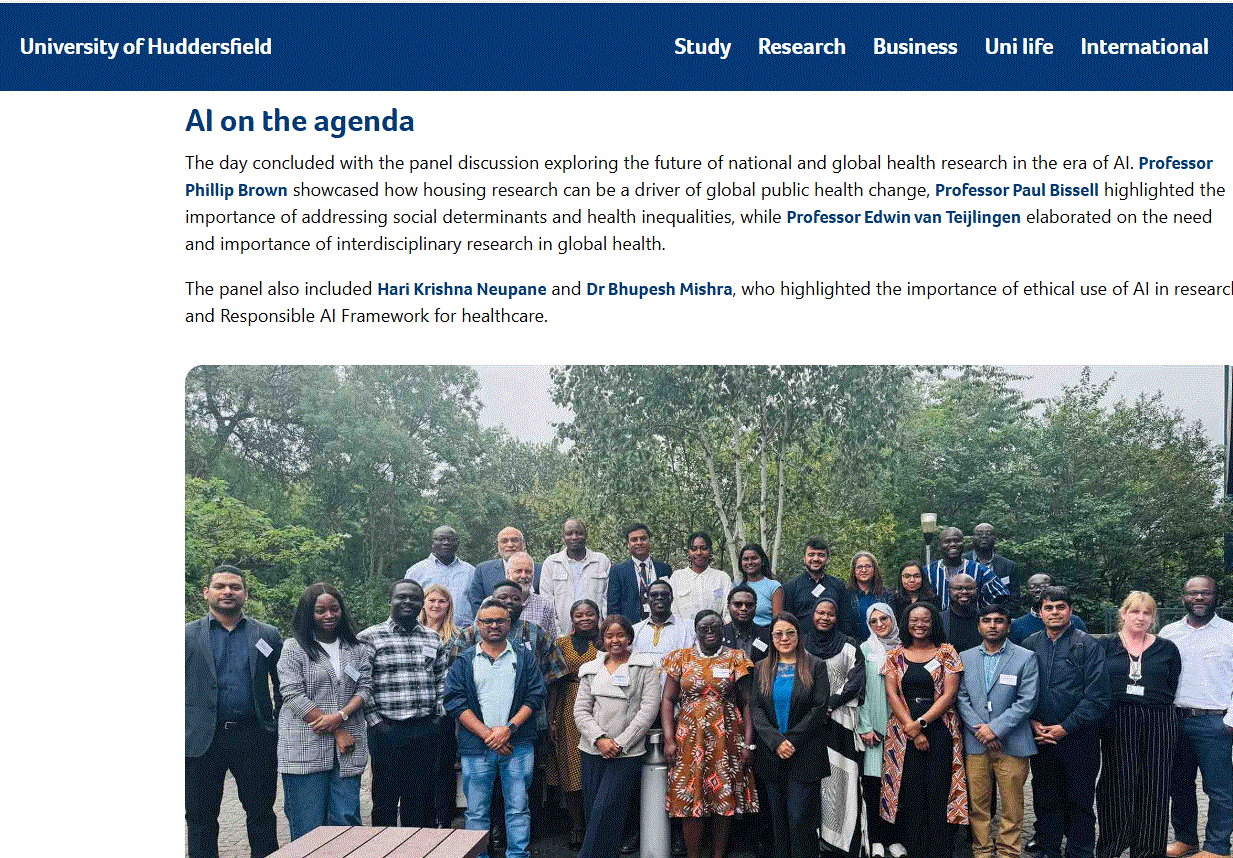
Today the University of Huddersfield reported online on the international array of over 70 delegates who attended the Annual Meeting of the Global Consortium for Public Health Research (GCPHR) hosted by the University of Huddersfield in June. Academics, policymakers, clinicians and researchers from around the world (including from Bournemouth University) spent two days on campus for the third GCPHR yearly meeting. Further details on the online report can be read here!
Prof. Edwin van Teijlingen
Centre for Midwifery & Women’s Health













 Opportunities to support our REF preparations
Opportunities to support our REF preparations SPROUT Returns: Designing Sustainability in Research Practice – Wednesday 20 May 12-2pm
SPROUT Returns: Designing Sustainability in Research Practice – Wednesday 20 May 12-2pm Innovative Approaches to Doctoral Supervision: Selected Case Studies
Innovative Approaches to Doctoral Supervision: Selected Case Studies 3C Event: Research Culture, Community & Canapés-Tuesday 19 May 1-2pm
3C Event: Research Culture, Community & Canapés-Tuesday 19 May 1-2pm New chapters published in maternity book on risk
New chapters published in maternity book on risk Apply now to take part in the 2026 ESRC Festival of Social Science
Apply now to take part in the 2026 ESRC Festival of Social Science Reminder: Register for the ESRC Festival of Social Science 2026 Information Session
Reminder: Register for the ESRC Festival of Social Science 2026 Information Session ECR Funding Open Call: Research Culture & Community Grant – Apply now
ECR Funding Open Call: Research Culture & Community Grant – Apply now ECR Funding Open Call: Research Culture & Community Grant – Application Deadline Friday 12 December
ECR Funding Open Call: Research Culture & Community Grant – Application Deadline Friday 12 December MSCA Postdoctoral Fellowships 2025 Call
MSCA Postdoctoral Fellowships 2025 Call ERC Advanced Grant 2025 Webinar
ERC Advanced Grant 2025 Webinar Update on UKRO services
Update on UKRO services European research project exploring use of ‘virtual twins’ to better manage metabolic associated fatty liver disease
European research project exploring use of ‘virtual twins’ to better manage metabolic associated fatty liver disease