Worldwide there is a growing interest in interdisciplinary research, especially to help deal with large questions in life, the so-called wicked problems. These wicked problems (or questions) include climate disasters and global warming, globalisation, the drop in biodiversity, inequalities and international conflicts. Interdisciplinary research increasingly popular and widely promoted by grant-giving bodies, the UK REF (Research Excellence Framework), research councils and universities, to name but a few stakeholders.
However, it is often ignored, that interdisciplinary research presents significant challenges for discipline-specific experts. Doing interdisciplinary research requires specialised skills, team-player personality traits, and the ability to transcend one’s own academic boundaries. We have highlighted in the past that common barriers include managing conflicting research philosophies, navigating, and overcoming, methodological, and communication differences [1]. Those who have been involved in interdisciplinary research will agree that is not an easy option for the individual discipline expert. It requires individual skills, ability to see beyond one’s discipline and perhaps personality characteristics such as a great team player. Interdisciplinary research may involve a mixed-methods approach underpinned by conflicting, and according to some incommensurable, research philosophies.
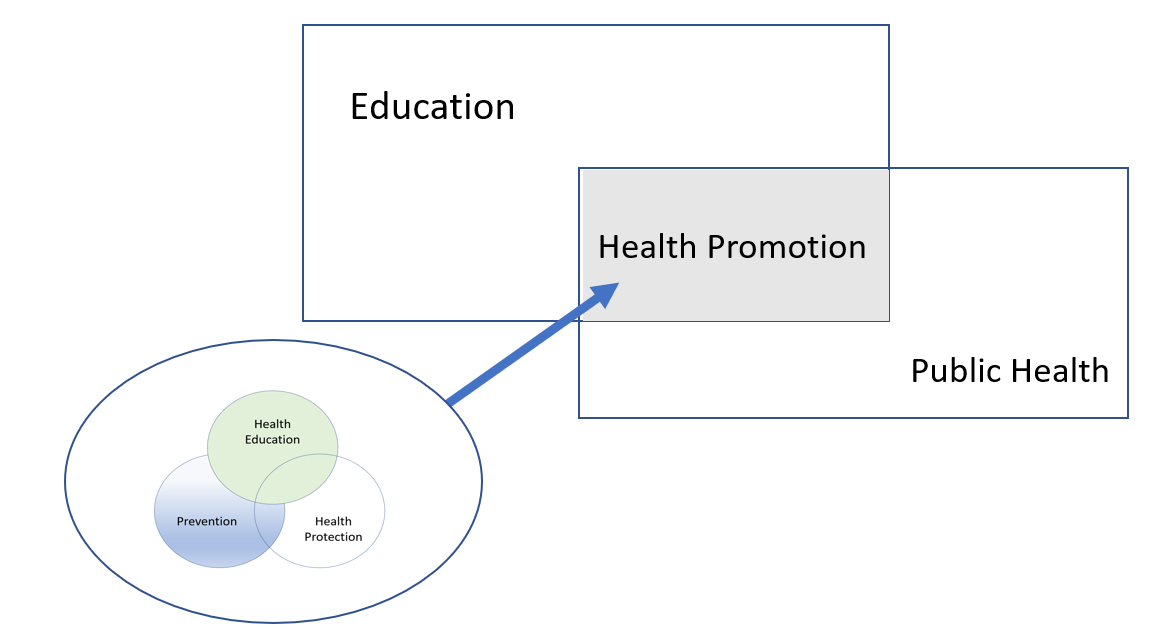
 It is also the case that some disciplines are perhaps more familiar with interdisciplinary working, disciplines such as Public Health [2] are traditionally less theory focused and more solution driven. But even in Public Health as a broad-ranging discipline covering sub-disciplines such as epidemiology, health education, law, management, health psychology, medical statistics, sociology of health & illness and a wide-range of research methods, conducting interdisciplinary research is not necessarily easy [3].
It is also the case that some disciplines are perhaps more familiar with interdisciplinary working, disciplines such as Public Health [2] are traditionally less theory focused and more solution driven. But even in Public Health as a broad-ranging discipline covering sub-disciplines such as epidemiology, health education, law, management, health psychology, medical statistics, sociology of health & illness and a wide-range of research methods, conducting interdisciplinary research is not necessarily easy [3].
Prof. Edwin van Teijlingen & Dr. Pramod Regmi both are in the School of Health & Care, and Dr. Shanti Farrington, who is based in the School of Psychology.
References:
- Shanker S, Wasti SP, Ireland J, Regmi PR, Simkhada PP, van Teijlingen E. (2021) The Interdisciplinary Research Team not the Interdisciplinarist. Europasian Journal of Medical Science. 3(2):111-5.
- Wasti, S. P., van Teijlingen, E., Simkhada, P. (2020) Public Health is truly interdisciplinary. Journal of Manmohan Memorial Institute of Health Sciences, 6(1):21-22.
- van Teijlingen, E., Regmi, P., Adhikary, P., Aryal, N., Simkhada, P. (2019). Interdisciplinary Research in Public Health: Not quite straightforward. Health Prospect, 18(1), 4-7. https://doi.org/10.3126/hprospect.v18i1.19337












































 Art and Design: History, Practice and Theory academics – would you like to get more involved in preparing our next REF submission?
Art and Design: History, Practice and Theory academics – would you like to get more involved in preparing our next REF submission? UKCGE Recognised Research Supervision Programme: Final Deadline Reminder
UKCGE Recognised Research Supervision Programme: Final Deadline Reminder The significance of Rights and Protocols in Disaster Response
The significance of Rights and Protocols in Disaster Response Celebrate World Wellbeing Week This June
Celebrate World Wellbeing Week This June Official book launch at Bournemouth University
Official book launch at Bournemouth University Take a Break: Join the Creative Wellbeing Event
Take a Break: Join the Creative Wellbeing Event Horizon Europe Cluster 3 (Civil Security for Society) 2026 Calls Now Open
Horizon Europe Cluster 3 (Civil Security for Society) 2026 Calls Now Open MSCA Doctoral Networks 2026 Call Information Webinar
MSCA Doctoral Networks 2026 Call Information Webinar ESRC Festival of Social Science 2026: Application Deadline Extended to Thursday 25 June 2026
ESRC Festival of Social Science 2026: Application Deadline Extended to Thursday 25 June 2026 Reminder: Register for the ESRC Festival of Social Science 2026 Information Session
Reminder: Register for the ESRC Festival of Social Science 2026 Information Session ECR Funding Open Call: Research Culture & Community Grant – Apply now
ECR Funding Open Call: Research Culture & Community Grant – Apply now ERC Advanced Grant 2025 Webinar
ERC Advanced Grant 2025 Webinar Update on UKRO services
Update on UKRO services European research project exploring use of ‘virtual twins’ to better manage metabolic associated fatty liver disease
European research project exploring use of ‘virtual twins’ to better manage metabolic associated fatty liver disease