This week the 3rd Annual Meeting of the Global Consortium for Public Health (GCPHR) takes place at the University of Huddersfield on June 25th-26th. GCPHR 2025 was attended by people involved in global health research from the UK, India, Nepal, Qatar, and Ghana. Building on the success of the 2023 inaugural two-day meeting and the second annual event in 2024, the 2025 meeting brought together a diverse community of health researchers, practitioners, policy-makers and global health leaders. This initiative has as its main aim to facilitate the exchange of knowledge, promote innovation, and strengthen international collaboration.
 Bournemouth University academics have been involved since GCPHR’s inception, and this year Prof. Edwin van Teijlingen from the Centre for Midwifery & Women’s Health (CMWH) contributed to a panel discussion on ‘Innovating Tomorrow: National and Global Research in the Age of AI’. He presented around the pros and cons of Interdisciplinary Research in Global Health. Together with colleagues Edwin has published several papers on interdisciplinary research [1-3] and collaborative writing of research output with a range of colleagues from different disciplines [4-5].
Bournemouth University academics have been involved since GCPHR’s inception, and this year Prof. Edwin van Teijlingen from the Centre for Midwifery & Women’s Health (CMWH) contributed to a panel discussion on ‘Innovating Tomorrow: National and Global Research in the Age of AI’. He presented around the pros and cons of Interdisciplinary Research in Global Health. Together with colleagues Edwin has published several papers on interdisciplinary research [1-3] and collaborative writing of research output with a range of colleagues from different disciplines [4-5].
Prof. Padam Simkhada from the University of Huddersfield (and Visiting Faculty in BU’s Faculty of Health & Social Sciences outlined the recently awarded British Academy grant on ‘Evidence-based Policy-Making in Nepal’. The latter project, which includes BU’s Dr. Pramod Regmi as co-investigator, also has policy-makers in Nepal as collaborators, giving it great potential to become a REF Impact Case-Study.
References:
- Shanker, S., Wasti, S.P., Ireland, J., Regmi, P., Simkhada, P., van Teijlingen, E. (2021) The Interdisciplinary Team Not the Interdisciplinarist: Reflections on Interdisciplinary Research, Europasian Journal of Medical Sciences 3(2): 1-5. https://doi.org/10.46405/ejms.v3i2.317
- van Teijlingen, E., Regmi, P., Adhikary, P., Aryal, N., Simkhada, P. (2019). Interdisciplinary Research in Public Health: Not quite straightforward. Health Prospect, 18(1), 4-7. https://doi.org/10.3126/hprospect.v18i1.19337
- Wasti, S. P., van Teijlingen, E., Simkhada, P. (2020) Public Health is truly interdisciplinary. Journal of Manmohan Memorial Institute of Health Sciences, 6(1):21-22.
- Harvey, O., van Teijlingen, A., Regmi, P.R., Ireland, J., Rijal, A., van Teijlingen, E.R. (2022) Co-authors, colleagues, and contributors: Complexities in collaboration and sharing lessons on academic writing, Health Prospect 21(1):1-3. https://www.nepjol.info/index.php/HPROSPECT/article/view/39320/31432
- Hundley, V., Luce, A., Simkhada, P., van Teijlingen, E. (2022) Collaborative Writing for Publication, In: Wasti, S.P., et al. (Eds.) Academic Writing and Publishing in Health & Social Sciences, Kathmandu, Nepal: Himal Books: 15-19.



 Bartholomew V, Hundley V, Clark C, Parris B (2024) The RETHINK Study: Could pain catastrophisation explain why some women are more likely to attend hospital in early labour. Sexual & Reproductive Healthcare
Bartholomew V, Hundley V, Clark C, Parris B (2024) The RETHINK Study: Could pain catastrophisation explain why some women are more likely to attend hospital in early labour. Sexual & Reproductive Healthcare 





 Several midwives from the
Several midwives from the 
 The conference is a great opportunity for emerging researchers. Two of CMMPH postgraduate researchers had the opportunity to share their work with midwives from across the globe. Anna Marsh presented her recently completed MRes work titled ‘How do midwives portray birth on Instagram? A content analysis of posts from the USA, UK, New Zealand and Australia’.
The conference is a great opportunity for emerging researchers. Two of CMMPH postgraduate researchers had the opportunity to share their work with midwives from across the globe. Anna Marsh presented her recently completed MRes work titled ‘How do midwives portray birth on Instagram? A content analysis of posts from the USA, UK, New Zealand and Australia’. Vanessa Bartholomew, clinical academic doctoral midwife, presented ‘The RETHINK Study: A study to determine if pregnant women who pain catastrophise are more likely to attend hospital during the latent phase of labour’. We are very proud to say that Vanessa’s poster won the conference competition for ‘Best Scientific Poster’!
Vanessa Bartholomew, clinical academic doctoral midwife, presented ‘The RETHINK Study: A study to determine if pregnant women who pain catastrophise are more likely to attend hospital during the latent phase of labour’. We are very proud to say that Vanessa’s poster won the conference competition for ‘Best Scientific Poster’! This has been a busy few months for the International Early Labour Research Group (IELRG), which comprises members from across the globe. We had the opportunity to get together at the International Labour and Birth Research Conference in Grange over Sands this month, where early labour was a strong theme.
This has been a busy few months for the International Early Labour Research Group (IELRG), which comprises members from across the globe. We had the opportunity to get together at the International Labour and Birth Research Conference in Grange over Sands this month, where early labour was a strong theme.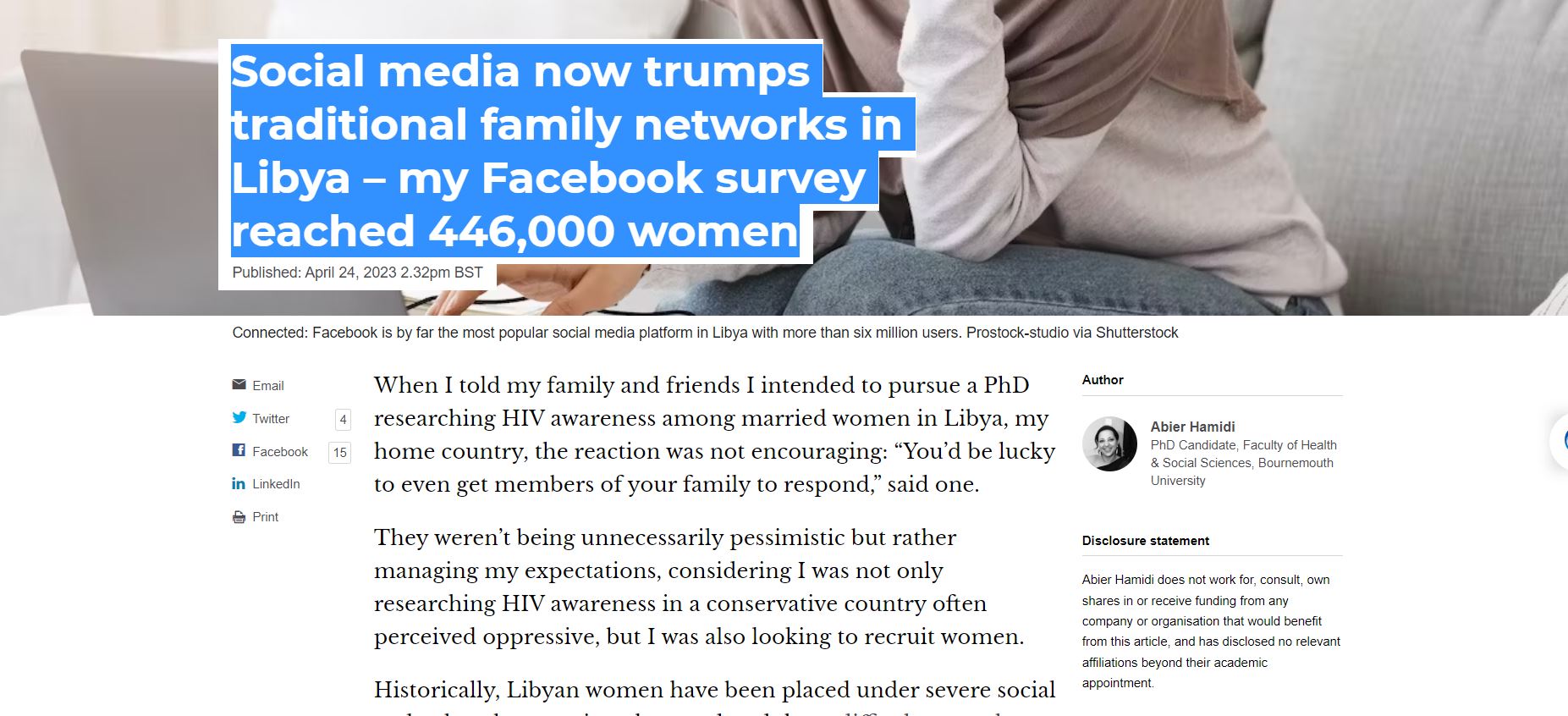


































 BU students’ publishing success
BU students’ publishing success BU presentation at the University of Bristol
BU presentation at the University of Bristol Art and Design: History, Practice and Theory academics – would you like to get more involved in preparing our next REF submission?
Art and Design: History, Practice and Theory academics – would you like to get more involved in preparing our next REF submission? UKCGE Recognised Research Supervision Programme: Final Deadline Reminder
UKCGE Recognised Research Supervision Programme: Final Deadline Reminder The significance of Rights and Protocols in Disaster Response
The significance of Rights and Protocols in Disaster Response Celebrate World Wellbeing Week This June
Celebrate World Wellbeing Week This June Horizon Europe Cluster 3 (Civil Security for Society) 2026 Calls Now Open
Horizon Europe Cluster 3 (Civil Security for Society) 2026 Calls Now Open MSCA Doctoral Networks 2026 Call Information Webinar
MSCA Doctoral Networks 2026 Call Information Webinar ESRC Festival of Social Science 2026: Application Deadline Extended to Thursday 25 June 2026
ESRC Festival of Social Science 2026: Application Deadline Extended to Thursday 25 June 2026 Reminder: Register for the ESRC Festival of Social Science 2026 Information Session
Reminder: Register for the ESRC Festival of Social Science 2026 Information Session ECR Funding Open Call: Research Culture & Community Grant – Apply now
ECR Funding Open Call: Research Culture & Community Grant – Apply now ERC Advanced Grant 2025 Webinar
ERC Advanced Grant 2025 Webinar Update on UKRO services
Update on UKRO services European research project exploring use of ‘virtual twins’ to better manage metabolic associated fatty liver disease
European research project exploring use of ‘virtual twins’ to better manage metabolic associated fatty liver disease