 Yesterday the Nepal Journal of Epidemiology published our editorial on ‘Strengthening Healthcare through Academic and Industry Partnership Research’ [1]. The editors put the editorial on the cover of the latest issue of the journal. Academic and Industry Partnership Research can drive medical innovation, strengthen patient-centred research, and close the gap between theoretical understanding and real-world implementations. The UK’s dedication to developing long-term alliances based on mutual respect and open dialogue can facilitate an environment where ground-breaking research can flourish and be transformed into affordable health and social care solutions.
Yesterday the Nepal Journal of Epidemiology published our editorial on ‘Strengthening Healthcare through Academic and Industry Partnership Research’ [1]. The editors put the editorial on the cover of the latest issue of the journal. Academic and Industry Partnership Research can drive medical innovation, strengthen patient-centred research, and close the gap between theoretical understanding and real-world implementations. The UK’s dedication to developing long-term alliances based on mutual respect and open dialogue can facilitate an environment where ground-breaking research can flourish and be transformed into affordable health and social care solutions.Half of the authors are associated with Bournemouth University, two are Visiting Faculty (Prof. Dr. Padam Simkhada and Dr. Brijesh Sathian) and the third one is Prof. Edwin van Teijlingen in the Centre for Midwifery & Women’s Health (CMWH). The Nepal Journal of Epidemiology is an Open Access journal and therefore the paper is freely available to read to anyone across the globe.
References:
- Sathian, B., van Teijlingen, E. ., Simkhada, P., Banerjee, I., Manikyam, H. K., & Kabir, R. (2023). Strengthening Healthcare through Academic and Industry Partnership Research. Nepal Journal of Epidemiology, 13(2), 1264–1267. https://doi.org/10.3126/nje.v13i2.58243




















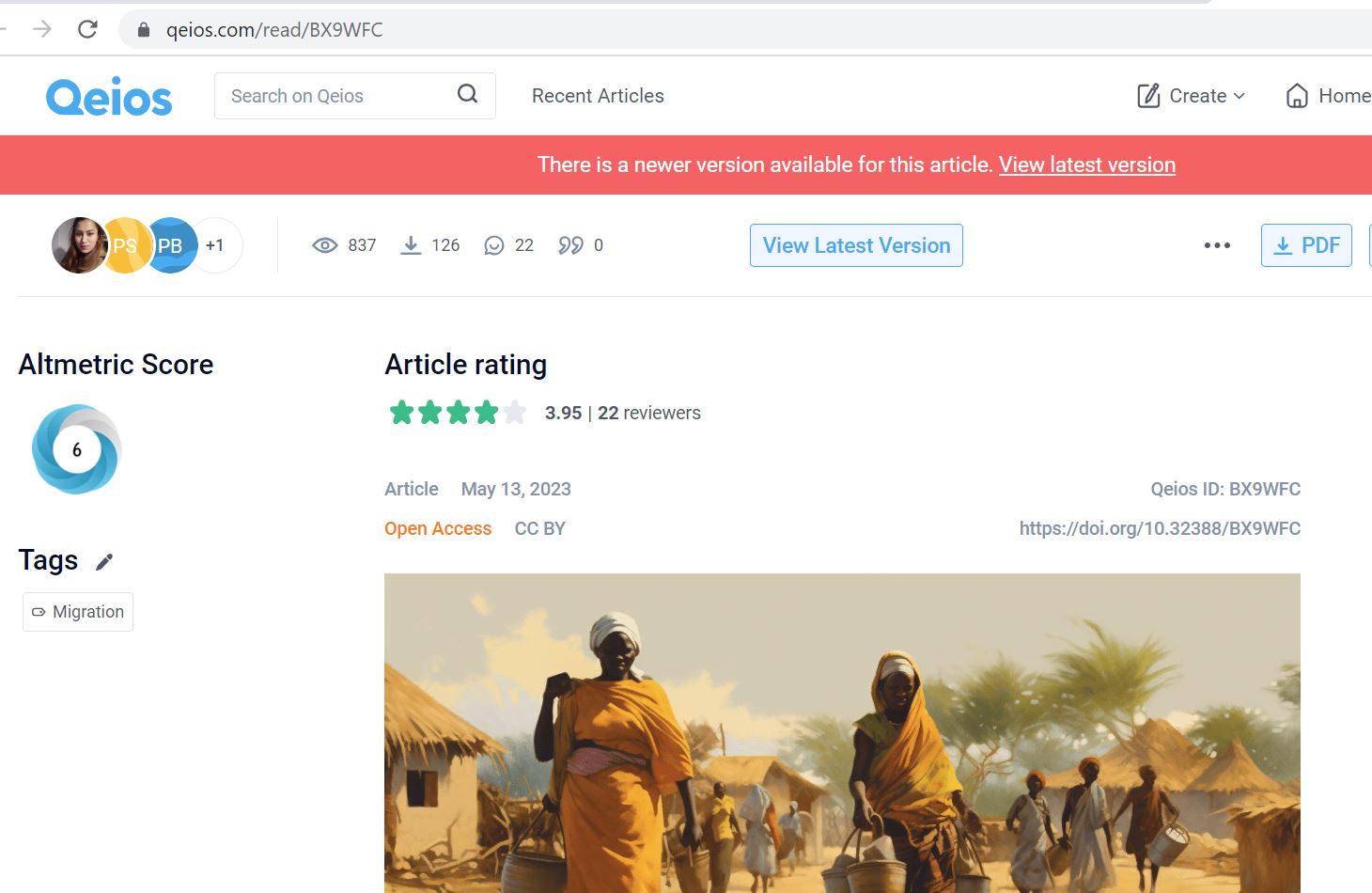









 Last we took a new step into the academic publishing by submitting a paper to Qeios. This Open Access journal publishes papers for free, more or less immediately and after the paper has appeared online peer-reviewers are being invited. The paper ‘
Last we took a new step into the academic publishing by submitting a paper to Qeios. This Open Access journal publishes papers for free, more or less immediately and after the paper has appeared online peer-reviewers are being invited. The paper ‘











 REF mock exercise 2026 – nominate your research outputs on BRIAN
REF mock exercise 2026 – nominate your research outputs on BRIAN ESRC Festival of Social Science 2026: Application Deadline Extended to Thursday 25 June 2026
ESRC Festival of Social Science 2026: Application Deadline Extended to Thursday 25 June 2026 First publication for two CMWH PhD students
First publication for two CMWH PhD students SPROUT Returns: Designing Sustainability in Research Practice – Wednesday 20 May 12-2pm
SPROUT Returns: Designing Sustainability in Research Practice – Wednesday 20 May 12-2pm Reminder: Register for the ESRC Festival of Social Science 2026 Information Session
Reminder: Register for the ESRC Festival of Social Science 2026 Information Session ECR Funding Open Call: Research Culture & Community Grant – Apply now
ECR Funding Open Call: Research Culture & Community Grant – Apply now ECR Funding Open Call: Research Culture & Community Grant – Application Deadline Friday 12 December
ECR Funding Open Call: Research Culture & Community Grant – Application Deadline Friday 12 December MSCA Postdoctoral Fellowships 2025 Call
MSCA Postdoctoral Fellowships 2025 Call ERC Advanced Grant 2025 Webinar
ERC Advanced Grant 2025 Webinar Update on UKRO services
Update on UKRO services European research project exploring use of ‘virtual twins’ to better manage metabolic associated fatty liver disease
European research project exploring use of ‘virtual twins’ to better manage metabolic associated fatty liver disease