Peer review is the the key pillar of academic publishing. Peer reviewers will read the submitted paper and assess its knowledge contribution, the appropriateness of the research question, the ethical considerations, the quality of the research methods used and the appropriateness of the discussion, conclusion, and recommendations in the manuscript. [1] It is worth bearing in mind that most peer reviewers are unpaid volunteers, academics like us who review for journals over and above the day job.[2] For the authors peer reviewers can give excellent feedback. Harvey and colleagues remind their readers that peer reviewers reading your manuscript with a fresh pair of eyes, can lead to them raising great questions and offering useful comments. In short, reviewers’ reservations and misunderstandings can help you to rephrase and better focus your paper. [3]
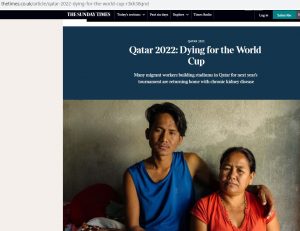
However, what the review process does not do is picking up every possible minor mistake and typo in a paper. I was reminded of this last week when I read a peer-reviewed paper in which the basic demographics table (the characteristics of the study participants) did not add up to 100%. Luckily, the same authors (who shall remain nameless) published a different paper from the same study in another quality journal, which allowed me to check the numbers. Interestingly, the second paper in another peer-reviewed journal had the same mistake. In the end I ended up writing to two different editors pointing out this anomaly. The editors contacted the authors who have since promised to rectify the mistake.
 Something similar has also happened to us. Occasionally I reread one of our articles in a good journal and wonder about some of the unclear sentences or poorly expressed grammar or style. Neither the editor nor the peer-reviewers spotted it nor did my co-authors and I noticed these mistakes in the paper proofs.
Something similar has also happened to us. Occasionally I reread one of our articles in a good journal and wonder about some of the unclear sentences or poorly expressed grammar or style. Neither the editor nor the peer-reviewers spotted it nor did my co-authors and I noticed these mistakes in the paper proofs.
Prof. Edwin van Teijlingen
CMMPH (Centre for Midwifery, Maternal & Perinatal Health)
References:
- van Teijlingen, E., Simkhada, P., Shanker, S. (2022) Selecting an Appropriate Journal and Submitting your Paper, In: Wasti, S.P., et al. (Eds.) Academic Writing and Publishing in Health & Social Sciences, Kathmandu, Nepal: Himal Books: 20-31.
- van Teijlingen, E., Thapa, D., Marahatta, S.B., Sapkota, J.L., Regmi, P. Sathian, B. (2022) Editors and Reviewers: Roles and Responsibilities, In: Wasti, S.P., et al. (Eds.) Academic Writing and Publishing in Health & Social Sciences, Kathmandu, Nepal: Himal Books: 32-37.
- Harvey, O., Taylor, A., Regmi, P.R., van Teijlingen, E. (2022) Struggling to reply to reviewers: Some advice for novice researchers. Health Prospect, 21(2):19-22.







































 ESRC Festival of Social Science 2026: Application Deadline Extended to Thursday 25 June 2026
ESRC Festival of Social Science 2026: Application Deadline Extended to Thursday 25 June 2026 First publication for two CMWH PhD students
First publication for two CMWH PhD students Opportunities to support our REF preparations
Opportunities to support our REF preparations SPROUT Returns: Designing Sustainability in Research Practice – Wednesday 20 May 12-2pm
SPROUT Returns: Designing Sustainability in Research Practice – Wednesday 20 May 12-2pm Innovative Approaches to Doctoral Supervision: Selected Case Studies
Innovative Approaches to Doctoral Supervision: Selected Case Studies Reminder: Register for the ESRC Festival of Social Science 2026 Information Session
Reminder: Register for the ESRC Festival of Social Science 2026 Information Session ECR Funding Open Call: Research Culture & Community Grant – Apply now
ECR Funding Open Call: Research Culture & Community Grant – Apply now ECR Funding Open Call: Research Culture & Community Grant – Application Deadline Friday 12 December
ECR Funding Open Call: Research Culture & Community Grant – Application Deadline Friday 12 December MSCA Postdoctoral Fellowships 2025 Call
MSCA Postdoctoral Fellowships 2025 Call ERC Advanced Grant 2025 Webinar
ERC Advanced Grant 2025 Webinar Update on UKRO services
Update on UKRO services European research project exploring use of ‘virtual twins’ to better manage metabolic associated fatty liver disease
European research project exploring use of ‘virtual twins’ to better manage metabolic associated fatty liver disease